What is Inclusion Body Myositis?
Inclusion Body Myositis (IBM) is a condition that causes muscles to become thin and weak. Symptoms usually start in middle to late life, and it is considered one of the most common muscle diseases diagnosed after the age of 50. Nevertheless, it is still regarded as rare, with between 3 and 4 people out of every 100,000 people over 50 having the condition.
The primary cause of IBM is currently unknown. There are likely a number of factors at play. Research suggests that there are both inflammatory and degenerative components of the disease. However, it remains unclear whether IBM is a primary, muscle-specific autoimmune disease or if it is a degenerative muscle disorder with an immune-inflammatory response.
IBM is not thought to be an inheritable genetic condition. It seems to occur with no discernible pattern. For this reason, it is often called sporadic IBM or sIBM. However, research indicates that genetic factors may make some people more vulnerable to developing IBM.
Notwithstanding, IBM is distinct from the Hereditary Inclusion Body Myopathies (hIBM). These are a group of several separate, very rare genetic disorders which have been linked to specific genetic causes. Like IBM, hIBMs cause muscle weakness, but inflammation is not a primary symptom.
Symptoms
- Slowly progressing muscle weakness
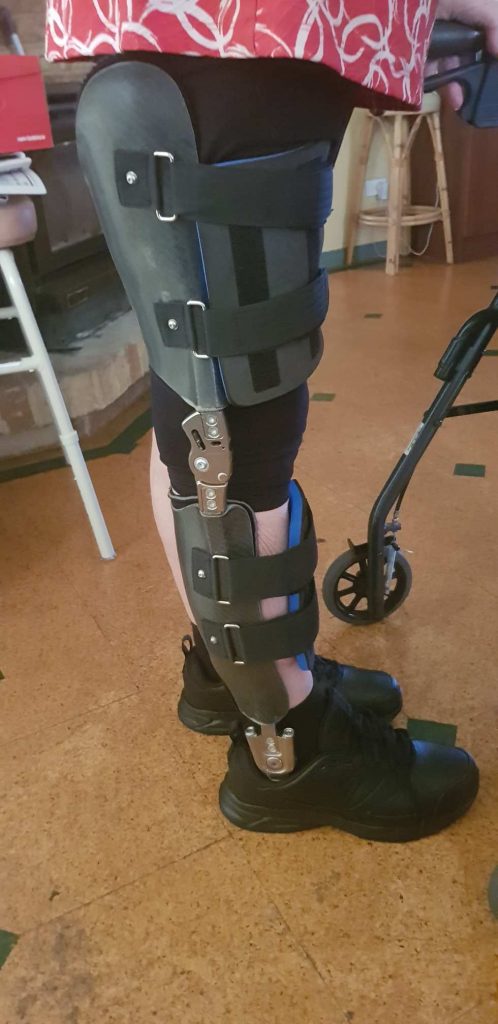
- Wasting in the arms and legs. Quadriceps (the main muscles of the thighs) are usually affected first leading to frequent falls
- Trouble climbing stairs
- Difficulty getting off the floor
- Difficulty with standing from a seated position
- Difficulty rolling over and getting out of bed
- Weakened forearm muscles that flex the fingers and wrists lead to a weakened hand grip. Over time, people may experience very significant difficulty with gripping, lifting, using tools or household implements, and personal care difficulties
- Tripping can be a problem due to weakness of muscles below the knees
- Often one side of the body is more affected than the other
- Swallowing difficulties (dysphagia) are common.
Progression of weakness
The muscles of the heart, lungs, eyes, gut and bladder are usually not affected by IBM, and neither is the brain or sense of touch.
Recent research has shown that people with IBM can have a higher prevalence of arterial hypertension leading to heart disease.
Speech is not typically affected, but changes in facial muscles may occur.
Pain or discomfort and fatigue may be experienced as muscles weaken, though often patients report no pain.
Most meet with some degree of disability as the disease progresses. Research indicates that the average annual rate of muscle strength decline varies from 3–15%. Walking and basic daily routines progressively become more difficult, leading to the need for assistive technology and possibly a wheelchair, 10 to 15 years after the onset of symptoms.
There’s currently no cure for IBM. While people can live long lives, it also can have fatal complications due to aspiration pneumonia in patients with dysphagia or respiratory failure due to a weak diaphragm or injuries from falls.
It has been noted that people with IBM are more likely to also have other medical conditions such as lupus (SLE), Sjögren’s syndrome, mitochondrial disease, scleroderma, sarcoidosis, thyroid dysfunction, high blood pressure and diabetes.
What causes Inclusion Body Myositis?
The cause of IBM is not fully understood. Researchers think that there are two processes happening in the muscle at the same time causing the symptoms. One process is inflammation which damages the muscles. Viruses and autoimmunity have both been implicated in causing the inflammation. However, since treatment with anti-inflammatory medication generally does not improve the symptoms of IBM, something else must be going on.
More recently researchers have been studying degenerative processes occurring in the muscles of people with IBM. When viewed under a microscope, the muscle cells of people with IBM contain abnormal protein clumps called inclusion bodies, which give the condition its name. These clumps are thought to be toxic to the cell and cause them to deteriorate.
How these two processes of inflammation and degeneration interact, and if one causes the other is not yet fully understood.
See the recently published article McLeish E, Slater N, Sooda A, Wilson A, Coudert JD, Lloyd TE, Needham M.Inclusion body myositis: The interplay between ageing, muscle degeneration and autoimmunity. Best Pract Res Clin Rheumatol 2022 Jun 24:101761.doi:10.1016/i.berh.2022.101761 https://pubmed.ncbi.nlm.nih.gov/35760741/
How is Inclusion Body Myositis diagnosed?
IBM is thought to be underdiagnosed and frequently misdiagnosed as Polymyositis. It is also sometimes diagnosed as Motor Neurone Disease. So getting the correct diagnosis can be a long and frustrating process. Getting a diagnosis involves gathering various pieces of evidence that when put together point to IBM:
- Blood test: When muscles are damaged they release a protein into the blood stream called creatine kinase (CK). In some people with IBM the level of this protein in the blood can be moderately raised. For others, it can be normal or only slightly raised. Elevated CK levels may alert the physician to the possibility of muscle disease.
There is also a relatively new blood test that detects a certain antibody called ‘anti-cN1A’ or ‘anti-NT5C1A’ in the blood. The blood test comes back positive in about 50 percent of patients with IBM. This blood test is not strictly specific to IBM and can detect other autoimmune diseases. It is useful in helping to distinguish IBM from Polymyositis. However, this blood test may not be widely available yet.
- Electromyography (EMG): a test that assesses the electrical activity of the muscles and the nerves controlling the muscles. In IBM, abnormal electrical impulses may be detected. EMG may be helpful in confirming that a muscle disease is involved but it cannot make a definite diagnosis. Sometimes, the results may be misleading as they can also suggest the possibility of neurological disorders such as motor neurone disease.
- Muscle imaging: MRI or CT scans can show disease-specific patterns of muscle involvement associated with IBM. [EV5] This may help support a diagnosis of IBM and help distinguish it from other forms of Myositis.
- Muscle biopsy: The gold standard test for IBM is a muscle biopsy. The biopsy involves taking a small sample of muscle under general or local anaesthetic. This is examined under a microscope and different stains used to highlight different parts of the muscle. In IBM, muscle cells will contain inclusion bodies, which are abnormal clumps of proteins seen in damaged cells.
Because muscle weakness in IBM can progress slowly, a diagnosis is sometimes delayed for years after the onset of weakness. In some patients, the initial biopsy may give inconclusive results, and subsequent biopsy/ies may be necessary.
In other forms of myositis steroid treatment may be helpful. If steroids fail to help then this may give rise to consideration of IBM as a possible diagnosis.
How can the symptoms be managed?
There are currently no effective curative treatments for IBM but much can be done to manage the symptoms.
Immunosuppressive drugs such as corticosteroids may be helpful in other types of myositis but usually people with IBM do not see any improvement with these medications or if they do, the improvement is only short lived.
One study has even suggested that people with IBM who take immunosuppressive medication are actually worse off in the long term. In addition, unwanted side effects are possible, so these medications are not recommended. However, a trial of immunosuppressive therapy may be considered if a person has an atypical presentation of IBM or has another autoimmune disease.
Some people find Intravenous Immunoglobulin (IVIG) blood plasma therapy helpful in managing symptoms of dysphagia. This product is given as an infusion over several hours. Special authorisation from qualified doctors is required to access the product and should be discussed with medical specialists . More information on IVIG is available here.
For therapy that does not involve drugs, exercise may be beneficial for all people with IBM. Recent research has shown that regular exercise is generally helpful for people with IBM and may even modestly improve strength. Care must be taken to avoid falls and injuries though.
When undertaking a new exercise program it should be tailored for your ability and closely monitored by a health professional to avoid over exerting the muscles. If there is significant and long lasting muscle pain or weakness – you are probably overdoing it!
There is no specific exercise prescription for IBM but combining both aerobic and resistance exercise is generally recommended. For example, a short walking or swimming session one day and then the next day a short session of exercise using light weights. The exercise program could also include some hydrotherapy. Further research is ongoing to help to define the optimal exercise regime for people with IBM.
A physiotherapist or exercise physiologist can help maximise the efficiency of the relatively unaffected muscles. They can also advise on the use of walking aids and teach people how to transfer between chairs, beds and wheelchairs (if they become necessary). Advice on exercise to do at home may also be given.
Occupational therapists (OTs) can provide advice and equipment to assist in overcoming the everyday practical problems that people with IBM may face. Examples include cutlery with chunky handles to make gripping easier, aids to help stair climbing, ramps for entry to doors, walking aids, lifting chairs and advice on bathroom facilities.
Trouble swallowing may cause fragments of food or drink to enter the windpipe resulting in coughing after meals, chest infections and significant weight loss. Speech therapists can help with the management of swallowing difficulties if this develops. Occasionally minor surgery is performed to improve swallowing.
Keeping to an ideal weight is also advised because weakened muscles may struggle to carry excess weight.
Presently there is no scientifically recognised diet specific for people with IBM but research is underway. Balanced healthy diets which include high protein, vegetables and fruit, fats, fibre and low carbohydrate are suggested.of vegetables and two of fruit per day.
What research is being done?
Research is ongoing to learn more about IBM and test potential treatments.
ABC008 Immunotherapy
Researchers are currently recruiting Australian participants to take part in a phase 1 clinical trial that is part of a global study testing a new IBM treatment drug, ABC008. This drug has been designed to designed to reduce the number of specific, harmful immune cells attacking muscle cells in people living with IBM.
The Perron Institute in Western Australia is the first Australian recruiting site for the ABC008 trial. To learn more visit: https://www.perroninstitute.org/clinical-trials/myositis-trial/
Sirolimus (aka Rapamycin)
A global research team led by The University of Notre Dame Australia School of Medicine’s Professor Merrilee Needham, in collaboration with Perron Institute, Fiona Stanley Hospital and Murdoch University, is investigating the use of a re-purposed drug (Sirolimus) in the treatment of IBM.
Currently, the drug is primarily used to prevent organ rejection in post-kidney transplant patients. The research team hypothesise that Sirolimus will stabilise or slow disease progression over an 88-week trial period.
Sirolimus has been previously piloted in a small IBM cohort in France, with promising results. The Australian trial started in mid-2022. Sites are located in Perth, Adelaide, Melbourne, Sydney and Brisbane. Other sites overseas will be involved in the trial. Contact mail@myositis.org.au for more information.

Oxandrolone
One research strategy is to test drugs already in use for other conditions to see if they may also be useful for IBM. One such drug is oxandrolone which is an anabolic steroid that has the effect of building more muscle and increasing body weight.
A small trial of oxandrolone in 13 people with IBM showed some improvement in muscle strength, mainly upper body strength. However, further trials are needed to assess the benefits and risks of this drug for people with IBM.
Etanercept
A pilot trial of etanercept, a drug used to treat autoimmune diseases like rheumatoid arthritis, did not show significant benefit in muscle strength scores at six months. However, with 12 months of treatment, a slight improvement in grip strength was noted.
A larger clinical trial to assess the effectiveness of etanercept treatment for IBM in more detail was completed in 2014. However, no results for this study are available.
Alemtuzumab
There has been a small clinical trial involving 13 people with IBM. They were treated with alemtuzumab (Campath), a drug used to treat a type of leukaemia and multiple sclerosis (MS). This drug depletes the immune system of white blood cells. It was reported that disease progression was slowed, and strength improved in some patients. A larger placebo-controlled trial is now required to confirm this result and ensure that the risk of side effects does not outweigh the benefit.
Arimoclomol
Unfortunately, one new drug being developed for the treatment of IBM, arimoclomol, has failed to meet its primary and secondary endpoints in its phase 2/3 trial at 20 months. The company developing the drug announced these topline results in March 2021.
Bimagrumab
Another strategy for developing a treatment for IBM is to boost muscle growth. One way to do this is to interfere with the mechanisms naturally present in the muscle that put the brakes on muscle growth so that muscles remain within the normal size range. This involves a protein called myostatin, which inhibits muscle growth when it binds to certain receptors on the muscle. Interfering with this process could result in increased muscle growth and strength.
Drug company Novartis tested an investigational drug called BYM338 (also known as bimagrumab) for IBM. BYM338 is an antibody that binds to receptors on muscle, thereby blocking myostatin from binding to them.
A phase 2 clinical trial showed that BYM338 benefited patients with IBM compared to placebo. As such, an extension study was done. It indicated that while bimagrumab was well-tolerated, it did not appear to provide a clinical meaningful functional benefit compared with placebo. As a result, the study was cancelled early.
There was another extension study undertaken that involved 10 participants. The results noted an increase in muscle mass on a group level; however, there was no evidence of clinical improvement.
Follistatin Gene Therapy
Other researchers in the USA aim to inhibit the myostatin mechanism using a form of gene therapy. It involves increasing levels of a protein called follistatin, a natural myostatin inhibitor.
A harmless virus delivers the follistatin gene inside muscle cells, and these instructions are used to make the follistatin protein.
A phase 1 clinical trial of six IBM patients reported an improvement in the six-minute walking time test (used to evaluate walking capability). However, these trial result interpretations have been questioned, primarily based on the trial design.
Stay up to date
Research is moving forward at a fast pace, so this research summary may not be up-to-date at the time of reading. One of the best ways to stay up to date with the latest on research is to become a member. We regularly provide updates on research in our bi-monthly member newsletters.